Help is now just one (video) call away for staff at Children’s Minnesota Minneapolis hospital who have questions or need assistance caring for kids with diabetes. It’s called the Telebuddy program. This program was developed in partnership by Children’s nurses, our quality and safety team, and telehealth experts. It’s a new way to connect staff from our Minneapolis hospital to diabetes experts at our St. Paul hospital for insulin management support.
Two paths, one vision
Song Khang, RN, BSN, RN, CPN and a clinical educator in St. Paul, saw a need for her staff to ask questions and get advice from colleagues who are experts in diabetes management when caring for kids with the disease. She started a buddy program for fellow St. Paul nurses to call the diabetes floor with questions about insulin pumps, counting carbs and more diabetes-related topics. While attending the Magnet® conference in 2018, Khang had an idea – what if we could start a telehealth buddy program to provide support beyond St. Paul?
Children’s McNeely Pediatric Diabetes Center is located on our St. Paul campus and because of this, “St. Paul is where the majority of kids with diabetes are cared for at Children’s,” said Khang. “By partnering [with the Minneapolis campus], we could help reduce the potential for insulin overdose.”
After receiving support from nursing leadership, Khang reached out to Judy Wenzel, manager of telehealth at Children’s, to begin exploring options. After that, Bobbie Carroll, RN, vice president of quality, heard about Khang’s vision and joined together to form an interdisciplinary work group. From there, the Telebuddy concept was born.
With the project management skills of Jessica Zeirke, BSBME, LSSBB, CQIA, quality and safety improvement consultant, the team secured iPads and equipment for the video calls, developed documentation and created an education plan. Throughout the process, the team paused and took time to listen and gather feedback from font-line staff.
“The Telebuddy project was a cross-functional effort and the shared ownership made an impact in its success,” said Cassie Johnson, MSN, RN, CNL, CPHON, a quality and patient safety coach. “The input we received from the nursing community council and unit councils along the way helped us evolve our approach so we could develop something that would work at the bedside.”
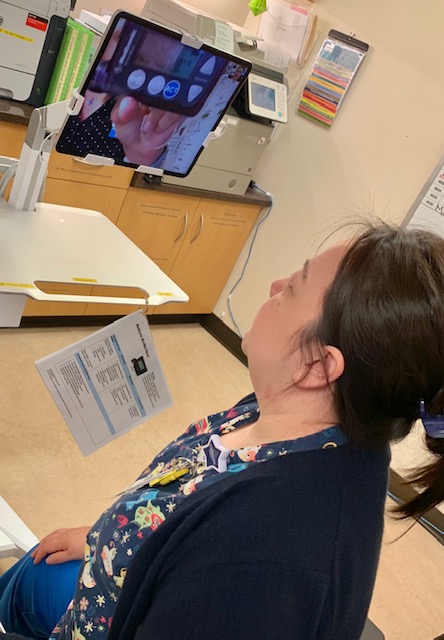
Telebuddy to the rescue
Since Telebuddy efforts began in September, there have already been more than 20 connections made between the campuses. Here’s how it works: A Minneapolis nurse with a question about a pump, insulin orders, medication or any other insulin management-related question, can connect with a St. Paul Telebuddy, which is the unit charge nurse. Via phone or video conference, they can have a real-time discussion and analysis of the situation to ensure the best outcome for patients.
Erin Januschka, BAN, RN, CPN, clinical educator in Minneapolis, is also grateful for the connection to their buddies in St. Paul.
“It’s a great system to have in place for those times when you need an answer quickly,” said Januschka. “Often times, our patients and their families know how to use their pumps, but when a patient is sedated or parents aren’t around, having the iPads and a Telebuddy can be a really helpful resource.”
Next steps
As use of the Telebuddy program continues to increase, so will staff comfort with insulin management. The quality and safety team plans to resurvey the staff working on the diabetes floors of our Minneapolis hospital in the future to measure the program’s success. In addition, the team is looking at additional ways to leverage telehealth throughout Children’s, for uses such as wound care or port-a-cath access.
“Telebuddy has been a great way to bring nurses from both sides of the river together,” said Natalie Lu, BA, MSN, RN, quality and patient safety coach. “The use of this technology has enabled us to not only reduce potential harm to patients, but also enabled us to become a stronger team.”