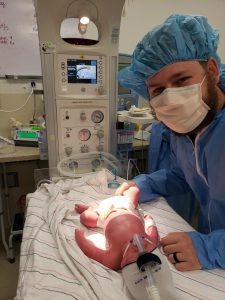
Michaela and Nic were excited to welcome their first baby, Xander. The pregnancy was going smoothly. Michaela never had morning sickness or pain. That changed when she had a growth scan at 32 weeks.
Her baby’s heart rate was up to 289 beats per minutes. A normal baby’s heart rate is between 110 and 180. Only a week before Christmas, Michaela was told her baby was in heart failure and she needed to get to the hospital that provided expert fetal and neonatal he needed.
Referral and diagnosis
Michaela’s obstetrician, Dr. Matthew Anderson at the AALFA Family Clinic, referred her to Midwest Fetal Care Center (MWFCC) in Minneapolis, a collaboration between Allina Health and Children’s Minnesota that brings together a multi-disciplinary team of experts from both health systems. Once Michaela arrived, she met Dr. Lisa Howley, medical director of fetal cardiology at Children’s Minnesota, and had an ultrasound where they could hear the baby’s heart beat was not normal.

Dr. Howley diagnosed unborn Xander with fetal supraventricular tachycardia (SVT), a type of abnormal heart rhythm where the heart beats very quickly. Making the situation more complicated, Xander also had hydrops – a life-threatening condition in which abnormal amounts of fluid accumulate in two or more body areas – indicating that his SVT had made him very sick. The couple was told that if Michaela delivered that day, their baby had less than a 50% chance of survival.
“It was very scary. It was a lot of unknown and completely unexpected because I had a super easy pregnancy up until then,” remembered Michaela.
Treatment plan for baby and mom
Michaela was admitted to The Mother Baby Center only days before the Christmas holiday. To try and get Xander out of SVT as fast as possible, Dr. Howley recommended treating him while still in the womb with an injection of heart rhythm medication directly into his arm through Michaela’s abdomen. In addition, Michaela began taking heart rhythm medications in order for them to cross the placenta to Xander and bring down his heart rate. After a few days, Xander’s heart was out of SVT!
“We chose to trust Dr. Howley because we could tell she was going to fight for our baby as much as we are,” said Michaela. “We knew if we didn’t do anything, we weren’t going to leave the hospital with him.”
Xander improved so much that Michaela was discharged from the hospital. But, just a couple days later she was readmitted for preeclampsia. The good news was Xander’s hydrops and heart rate were improving. Dr. Howley told the couple that if they gave birth, their son would be OK. One day later, that’s what happened. “He must have known and said, ‘OK, here I come!” said Michaela.
Delivery
Despite Xander’s improved medical condition, he arrived about six weeks early. After Michaela held him on her chest for a few seconds, Nic cut the umbilical cord and went with their son to the nearby neonatal intensive care unit (NICU) at Children’s Minnesota.
In the NICU, the team put Xander on a machine for breathing support. But he didn’t need it very long. After about 10 hours he was breathing room air and had a normal heart rhythm! Mom, dad and baby Xander were together as a family five hours after he was born.

Xander kept improving too! He graduated from the NICU a few days later and was transferred to the Infant Care Center (ICC).
“We take care of many SVT families, but Xander was one of the sickest and most challenging and I am thrilled that our team was successful,” said Dr. Howley.
Xander was able to go home a few weeks later. He’s still on a heart rhythm medication, but is doing well and loves cuddling with his mom and dad.
One team for mom and baby
Michaela and Nic are grateful for the entire care team and they couldn’t imagine a better team to care for their son – from the doctors to the nurses.
“It’s not something we ever want any other parent or family to go through. But being at The Mother Baby Center and Children’s Minnesota NICU, we were definitely in the right place for him,” said Michaela.
Kid with Courage
Xander was featured as one of KTTC-TV’s Kids with Courage. Watch the story here.