Respiratory distress syndrome (infant)
What is infant respiratory distress syndrome?
Infant respiratory distress syndrome (RDS) is a lung condition causing breathing problems in newborn premature infants. Another name for this condition is hyaline membrane disease (HMD).
RDS is most common in premature infants who are 30 weeks gestation or younger. Because a baby's lungs are not needed for breathing until after birth, they are one of the last organs to fully develop. The more premature the birth, the less able your baby's lungs are to function well.
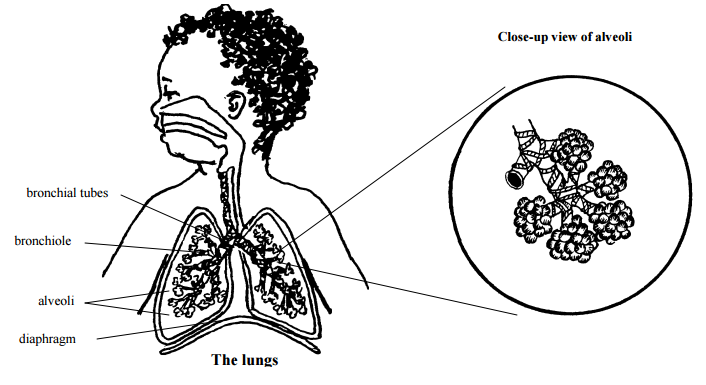
In the lungs, the exchange of oxygen and carbon dioxide takes place in the alveoli (small air sacs). Between the 24th and 26th weeks of pregnancy, the lungs begin to produce a substance called surfactant. Surfactant helps to keep the alveoli from collapsing once they are inflated.
A baby's first breath requires a big effort to open the alveoli and fill them with air for the first time. Without surfactant, each breath continues to require a great effort because the alveoli don't stay open. The infant soon tires and has trouble breathing.
After birth, the baby's lungs may take up to 5 days to produce surfactant.
What are the signs of RDS?
- breathing too fast or too slow
- flaring of the nostrils with breaths
- retractions (chest skin pulls in with breaths)
- chest may collapse with each breath
- grunting when breathing out
- skin color may be pale, bluish, or gray
How is RDS diagnosed?
A chest X-ray and blood test are done to help the doctor make the diagnosis.
How is it treated?
Treatment will depend on how ill the infant is. Extra oxygen may be needed. A ventilator (breathing machine) may also be needed to deliver oxygen and help remove carbon dioxide from your baby's lungs.
A heart monitor will be used, and blood tests and chest X-rays will be done.
Artificial surfactant may be given in some situations to expand the lungs. See the education sheet "Surfactant."
As babies get better, they are weaned from the oxygen or ventilator over several days. Some infants may continue to need extra oxygen. Most infants are soon breathing on their own and doing well.
How long will it take for my baby to get well?
There are many reasons why some babies recover faster than others. Infants who are on ventilators for a long time may develop changes in their lungs. This may increase the time they need ventilator support. Other factors such as infection can also affect recovery. Each baby responds and recovers in a unique way.
Questions?
This sheet is not specific to your child but provides general information. If you have any questions, please ask the doctor or nurse.
Children's Hospitals and Clinics of Minnesota
Patient/Family Education
2525 Chicago Avenue South
Minneapolis, MN 55404
Last Reviewed 7/2015 © Copyright
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2024 Children's Minnesota
