Breast pumping when your baby is in the hospital
Article Translations: (Spanish)
After giving birth, your body is ready to produce milk when your breasts are stimulated. If your baby is unable to breastfeed, we will help you develop and maintain a good supply of breast milk. Start pumping as soon as possible after your baby's birth. If you wait, it may be harder to develop your supply.
How do I develop my milk supply?
- Use an electric breast pump and a double pumping kit.
- If you don't have an electric breast pump at home, check with your nurse.
- Follow the manufacturer's instructions, and ask the nurse if you need help.
- Before pumping, wash your hands to keep germs from getting into your milk.
- Before and during pumping, gently massage your breasts to help milk flow.
- Start your pump on low pressure. Gradually turn up the suction so that you feel a deep pulling sensation. The
highest setting may not be needed.
- Pumping should not hurt.
How often should I pump?
- For the first two weeks, pump every 2 to 3 hours during the day and at least once during the night. This is as often as your baby would breastfeed, about 8 to 10 times per day.
- The number of pumpings per 24 hours is most important, not the amount of time between. Each pumping signals your body to make more milk.
- In the first few days after birth, pump at least 10 to 15 minutes per breast.
- As you produce more milk, watch for it to slow down or stop. Then restart the pump to trigger another milk release and pump for another few minutes.
Empty your breasts each time. Empty breasts signal your body to make more milk; full breasts tell your body to make less.
What is "let-down"?
Let-down is when your breasts release milk in response to signals from your hormones and nervous system. Let-down is also called the "milk ejection reflex."
Relaxation is the key to let-down. It happens easier if you are not tired or stressed. Here are some ways to enhance let-down:
- A warm shower
- Warm packs on your breasts
- A comfortable place to pump: chair, couch or bed
- Pillows for good back support
- Supplies within easy reach
- A favorite non-alcoholic beverage
- Listen to relaxing music
- Look at your baby or baby's pictures
Where can I pump at the hospital?
- A breast pump is available in your baby's room.
- There are also breast-pumping rooms in some areas of the hospital. Ask your nurse for the location.
How much milk is enough?
- Your goal is 24 to 30 ounces per 24 hours.
- You should reach this amount by the time your baby is 2 to 3 weeks old.
- Write down your amounts so you will know when you've met your goal. (See below for a pumping log.)
How do I keep up my milk supply?
- After reaching your goal you may be able to pump less often and still maintain your supply. Try sleeping for one 5 to 6 hour stretch at night. If you can do this without too much breast fullness, you may be able sleep through the night.
- Watch your amounts, as pumping less often can cause decreased milk volume.
- Be sure to empty your breasts each time you pump.
- Studies show that skin-to-skin care increases breastfeeding success. Try to do it daily for 1-3 hours if your baby's condition allows.
How do I store my milk?
- Use your freshly pumped milk for the very next feeding when possible.
- If your baby will not use the milk within one hour, pour it into a fresh plastic container provided by the hospital.
- Label it with your baby's name, date, and time.
- Ask your nurse or the unit coordinator for labels printed with your baby's name, and check to make sure they are correct. This is important so staff can make sure they are giving the right milk to the right baby.
- Refrigerate milk if it will be used within 48 hours. If not, freeze it.
- Always store milk in the back of the freezer or refrigerator (where temperature is steadiest and coldest).
- When you bring milk to the hospital, keep it cool in a small cooler with ice or ice packs.
How long the milk is usable depends on where you store it.
| Milk stored here: |
is safe for: |
| Refrigerator |
48 hours (if fresh)
24 hours (if thawed)
|
|
Frost-free freezer that is part of your refrigerator
(around 24° F)
|
4 months |
| Deep freezer at 0° F |
up to one year |
Thawing and warming breast milk
- Thaw frozen milk using oldest first. Put the container in the refrigerator. Once all the ice crystals are melted, label with thawing date and time.
- Before feeding your baby, warm the milk in lukewarm water.
- Do not let water cover the lid.
- You may also use this method to thaw milk, but if you won't be using it right away, move it to the refrigerator while still cold, and label it.
- Do not thaw or warm breast milk in hot water or the microwave. This weakens the milk's infection-fighting properties and microwaving causes hot pockets that can burn your baby.
How should I clean the pump kit?
- Each pump kit comes with instructions for cleaning your pump and pump kit.
- Use only clean parts for each pumping to prevent germs from getting into the milk
- If using a pump that is used by others, clean the pump with disinfectant wipes before use. Wear disposable gloves to keep disinfectant off hands and breasts.
- Note: After pumping, let the pump run for a few minutes to dry the inside of the tubing.
Clean parts after every pumping session:
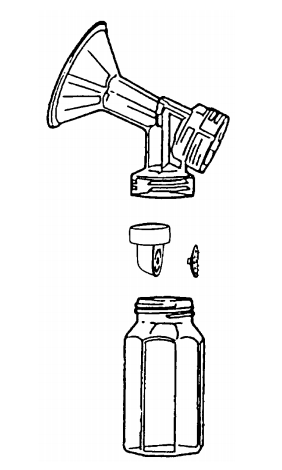
- Separate the parts that come in contact with the milk. If using the Medela® attachment kit, separate the yellow valve and white membrane.
- Rinse the parts in cool water to remove milk protein.
- Wash the parts in warm soapy water with a mild liquid detergent.
- Rinse in clear water.
- Air-dry on a clean towel or paper towels, covered with another towel. Ask your nurse for a plastic basin to wash and
store your pump kit parts.
- Sterilize pump parts daily by any of the following methods:
• Use Medela Quick-Clean bag
• Boil parts for 20 minutes
• Wash in dishwasher on sani-cycle
What else do I need to know?
- Pumping your breasts not only helps you make milk, it helps your uterus (womb) shrink and decreases bleeding.
- Get enough rest and stay healthy to keep up your milk supply.
- Eat a normal healthy diet. Your body may need up to 500 calories more per day than before you were pregnant. A sandwich and a glass of milk provide about 500 calories.
- Drink enough water to satisfy thirst. You are drinking enough if your urine is a light yellow.
- While bathing or showering wash your breasts with water only and pat dry. Avoid soap and lotion on your breasts; they tend to be drying or cause irritation.
- When your baby is ready to go home, ask the nurse to check the freezer for any of your milk so you can take it home.
When should I ask for help?
Ask your nurse if:
- You have breast pain
- Pumping hurts
- You are worried about your milk supply
Resources
Breast pumping log
Questions?
This is not specific to you and your baby but provides general information. If you have any questions while at Children's, please ask the nurse or lactation specialist:
Children's - Minneapolis 612-813-7654
Children's - St. Paul 651-220-7126
If you have any concerns after your baby goes home, make an appointment with your baby's doctor, nurse practitioner, or a lactation consultant.
La Leche League International is also available to provide help and support to breastfeeding mothers: 1-800-525-3243, www.llli.org
Back To Top
