September 2023 was a time of change for 14-year-old Peter. The teen had just started his freshman year of high school when he received alarming news – his eye doctor detected a slight problem in how his eyes move, which led to an MRI at Children’s Minnesota.
That’s when Peter’s family got the scary news. MRI scans revealed a large, slow-growing and non-cancerous brain tumor called a dermoid cyst. It filled the fluid spaces in his head – called ventricles – and was wrapped around critical brain structures, such as Peter’s thalamus which acts as a relay control center for almost everything in his body. The tumor also sat in the fornix that controls Peter’s memory and his ability to form new ones, and extended into his brainstem which controls vital functions. The dermoid likely started forming while Peter was in the womb.
“It didn’t sink in right away; it took a few days for the news to become real,” Peter said.
Additional concerns
The MRI also detected Peter had hydrocephalus. The large tumor acted like a dam and created buildup of cerebrospinal fluid (CSF) in the fluid places of his brain. Without surgery or treatment of the tumor, the hydrocephalus would have required surgery to place a special tube, called a shunt, from Peter’s brain to his abdomen to drain the CSF. Peter’s condition could have even led to a coma and possible death if left untreated.

Because of this, Peter was immediately admitted into our Minneapolis hospital for observation and eventual brain surgery.
“I felt OK and didn’t have any symptoms, so it took some time to accept and understand that I’d need a big surgery,” Peter said.
Developing a care plan
Peter’s family worked closely with The Kid Experts® in the Children’s Minnesota neurosurgery program, including neurosurgeon Dr. Amy Bruzek, to create a custom care plan. Because Peter had already developed hydrocephalus, Dr. Bruzek recommended immediate surgery.
“Dr. Bruzek answered every single question we ever had, and I never felt rushed or uninformed,” Peter’s mom, Melissa, said. “It felt like we were her only patients.”
Dr. Bruzek and her team explained to Peter and his family the tumor could not be completely removed because it surrounded and stuck to critical brain structures and large blood vessels. If they were damaged during surgery, it could be life-threatening. The neurosurgeon also explained other potential risks of removing the full tumor such as memory and cognitive deficits, or permanent weakness or numbness on one side of Peter’s body.
Preparing for brain surgery
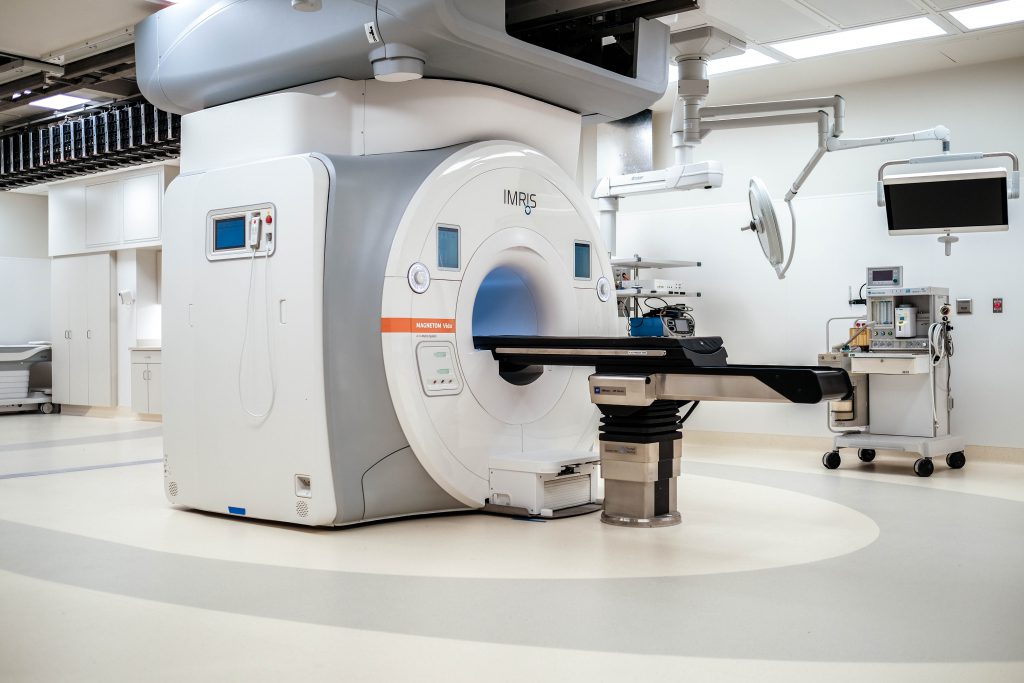
Peter was scheduled for brain surgery just 11 days after he first learned about his tumor. The procedure took place inside The Richard M. Schulze Family Foundation iMRI Surgical Suite. The state-of-the-art facility at our Minneapolis hospital is the first of its kind in North America, and it opened just six months before Peter learned about his diagnosis.
“I found it to be so comforting when I learned about the brand new iMRI suite, and how lucky we were to be in the first cohort of patients,” Melissa said.
The iMRI suite is a three-room surgery facility designed for our experts to seamlessly move a 16,200-pound MRI scanner directly into one of its operating rooms via a ceiling-mounted rail system. The Children’s Minnesota neurosurgery team and radiology department use the high-power scanner to take crystal-clear images mid-procedure.
This vital ability lets the care team confirm in real time if a tumor – or the parts of a tumor that can be safely removed – are out in a single surgery.
“The iMRI suite was so helpful in many ways, but the one thing I appreciate the most as a parent is that it allowed Peter to have only one surgery and recovery rather than possibly needing two separate surgeries,” Melissa said.
Peter’s procedure
Dr. Bruzek and her team performed a 12-hour craniotomy procedure. First, the neurosurgeon removed a small portion of Peter’s skull to create a temporary opening. The rest of the procedure was done endoscopically. Dr. Bruzek used a tiny video camera, called an endoscope, to see Peter’s tumor and surrounding brain tissue in his skull. The specialist then used small surgical instruments to safely remove at least 85% of the tumor.
“Doing this endoscopic procedure for such a large tumor was a big plus for Peter,” Dr. Bruzek said. “It can reduce the risk of post-surgery challenges, leaves a smaller incision and can help speed up recovery. I feel honored to be part of Peter’s care team.”
Dr. Bruzek said the procedure allowed her to correct Peter’s hydrocephalus without placing a shunt since the fluid buildup stopped on its own once most of the tumor was gone, and alternative routes were created for the fluid to flow.
Recovery and continued care
Peter spent more than a week recovering in our pediatric intensive care unit (PICU) and general surgery floor. His hospital team expanded to include physical and occupational therapy, child life and even a visit from the Minnesota Twins!
“The staff all cared for me and about me personally,” Peter shared. “They were willing to do whatever they could to be encouraging, supportive and help us get better as quickly as possible.”
Melissa said she always felt her family was in the absolute best care situation, “One of the many things that has really impressed me about Children’s Minnesota, besides exceptional medical care, is how thoroughly you care for the whole patient and even the family.”

Peter is now home, back in high school, and has routine follow-up appointments with our neurosurgery team. He’ll have MRIs and clinic visits throughout his life because the dermoid will likely continue to slowly grow, so he may have surgery again when he’s older.
Giving back to Children’s Minnesota
Peter served as a Star Gala Youth Ambassador to raise money and awareness for Children’s Minnesota and the 32nd annual Star Gala. This cherished annual event benefitted our neuroscience program in 2024.
“It was an honor to be able to give back, even a little bit, to the medical community that helped me so much,” Peter said. “I hope the staff know that they really make a difference to the kids they help.”