Translations available: Hmong, Spanish
A peak flow meter is a device that measures how well air moves out of the lungs. Many different types of meters are available.
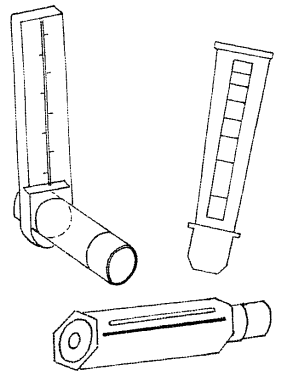
A peak flow meter is used to check your child's asthma, as a thermometer is used to check a temperature. During an asthma episode the airways in the lungs become narrow and the peak flow number may be low, showing that air is not moving easily through the lungs.
Using a peak flow meter can also help you and your child's doctor:
Be sure your child tries to do his or her best every time. The reading you see on the meter depends on your child's effort.
To use a peak flow meter your child should follow these steps:
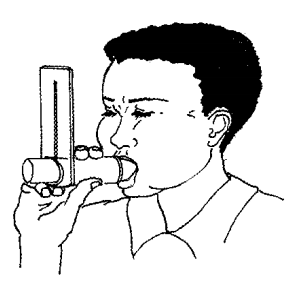
Your child's number can be determined from predicted normal peak flow values for people of the same age and height. See the chart at the end of this sheet for average peak flows for healthy children and teenagers.
Your health care professional can also determine your child's peak flow number based on a personal baseline. In this case your doctor will work with you to determine the peak flow numbers.
Once you know your child's predicted peak flow number, the doctor can use it to help put together an Asthma Action Plan. (See Asthma Action Plan.) The peak flow numbers on the Asthma Action Plan are set up like a traffic light. This will help you know what to do when your child's peak flow number changes.
Green Zone (80 to 100 percent of your child's predicted number) signals all clear. Your child is able to do usual activities and sleep without asthma symptoms such as cough, wheeze, shortness of breath, or chest tightness. Follow the Green Zone plan.
Yellow Zone (50 to 80 percent of your child's predicted number) signals caution. Your child has warning signs of an asthma episode that may include cough, wheeze, shortness of breath, chest tightness, or runny nose. Your child may have trouble sleeping through the night. Follow the Yellow Zone plan.
Red Zone (less than 50 percent of your child's predicted number) signals an emergency. Your child may have signs of difficult breathing, retractions (skin sucking in with each breath), trouble walking or talking, or the medicines may not be working. Follow the Red Zone plan.
This is not specific to your child but provides general information. If you have any questions, please call the clinic.
All tables are averages based on tests with a large number of people, and should be used as a guide only. Peak flows vary with the type of meter used.
| Height in inches | Average peak flow | Yellow Zone 50-80% of average peak flow |
Red Zone less than 50% of average peak flow |
| 43 | 147 | 74 - 118 | < 74 |
| 44 | 160 | 80 - 128 | < 80 |
| 45 | 173 | 87 - 139 | < 87 |
| 46 | 187 | 94 - 150 | < 94 |
| 47 | 200 | 100 - 160 | < 100 |
| 48 | 214 | 107 - 171 | < 107 |
| 49 | 227 | 114 - 182 | < 114 |
| 50 | 240 | 120 - 192 | < 120 |
| 51 | 254 | 127 - 203 | < 127 |
| 52 | 267 | 134 - 214 | < 134 |
| 53 | 280 | 140 - 224 | < 140 |
| 54 | 293 | 147 - 234 | < 147 |
| 55 | 307 | 154 - 246 | < 154 |
| 56 | 320 | 160 - 256 | < 160 |
| 57 | 334 | 167 - 267 | < 167 |
| 58 | 347 | 174 - 278 | < 174 |
| 59 | 360 | 180 - 288 | < 180 |
| 60 | 373 | 187 - 298 | < 187 |
| 61 | 387 | 194 - 310 | < 194 |
| 62 | 400 | 200 - 320 | < 200 |
| 63 | 413 | 207 - 330 | < 207 |
| 64 | 427 | 214 - 342 | < 214 |
| 65 | 440 | 220 - 352 | < 220 |
| 66 | 454 | 227 - 363 | < 227 |
Source: Polgar, G. and Promadht, V.: Pulmonary Function Testing in Children: Techniques and Standards, Philadelphia, WB Saunders Company, 1979.
Children's Hospitals and Clinics of Minnesota
ast reviewed 8/2015 © Copyright
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2026 Children's Minnesota