Epidural analgesia
What is epidural analgesia?
Analgesia means pain relief. The word epidural refers to a place in the back where the pain medicine is given. The medicine works directly on the nerves between the painful site and the brain.
Studies have shown that epidural analgesia provides excellent pain control for children. Compared to other methods of pain control, less pain medicine is usually needed when epidural analgesia has been used. Good pain control also promotes a faster recovery.
What does it look like?
A thin, very flexible tube will be inserted in your child's lower back next to the spinal cord by the anesthesiologist (anesthesia doctor) while your child is asleep. It is taped securely up the back and is connected to a pain medicine pump. The tape and connections will be checked by your nurse.
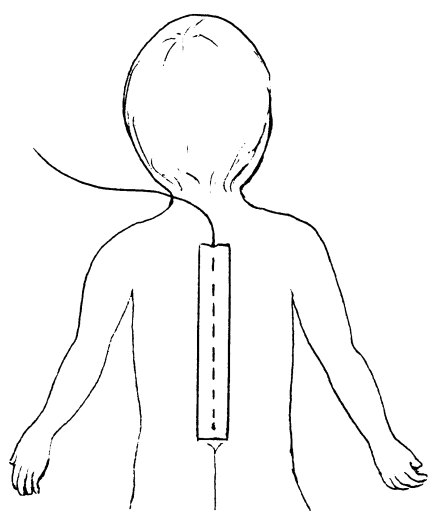
How does it work?
The pain medicine is given continuously and controlled by the pump. The medicine is pumped through the tube and comes out
next to the spinal cord, where it works on the nerves. A doctor prescribes the amount of pain medicine your child will receive. The nurse programs the pump so that the medicine will be given at the prescribed rate.
What are the side effects?
The most common side effect of pain medicines and anesthesia is drowsiness. Your child may sleep more than usual after surgery because of the pain medicine, and because sleep is the body's way of healing itself. The nurse will be checking to see how easily your child wakes up.
Other possible side effects are slow breathing, nausea (upset stomach), vomiting (throwing up), and itching. Medicines may be given to your child to help with any nausea, vomiting, or itching. Your child will be on monitors so that the nurses can watch the breathing rate and oxygen saturation.
Some children have numbness or tingling, especially in their legs. If your child has this feeling, tell your nurse. Although it is usually temporary, your nurse will check your child. A nurse will help your child the first time he or she gets out of bed. Sometimes a change in the medicine dose can decrease the numbness.
How can I help?
The nurses and doctors will ask you and your child how comfortable your child is. Because you know your child best, be sure to tell them if he or she seems uncomfortable to you. The nurses will also watch your child for signs of pain. They and the doctors will try to help your child be as comfortable as possible.
Children are usually on the epidural medicine for 2 to 5 days. Your nurses and anesthesiologist will talk to you and your child to find out if he or she is getting more comfortable each day after surgery. After the medicine pump is stopped, pain medicine is usually given by mouth.
Our commitment to pain management
We believe that infants, children, and teens have a right to the best level of pain relief that can be safely provided. Therefore, we take a team approach to pain and anxiety management, using drug and non-drug therapies. Our goal is to have staff and families work together to evaluate pain promptly and treat it effectively.
Questions?
This is not specific to your child, but provides general information. If you have any questions, please ask your doctor or nurse.
Last reviewed 8/2015
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2024 Children's Minnesota
