Breastfeeding an infant with neurological problems
How does breastfeeding help my baby?
Breast milk:
- is more nutritious and easier to digest than formula
- gives immune protection not found in formula
- lowers risk of infections
- helps minimize allergies
- helps the digestive system mature; protects against some bowel problems
- lowers risk of Sudden Infant Death Syndrome (SIDS)
- promotes eye and brain development
- is more economical than formula
When you breastfeed:
- you create a special bond with your baby
- your baby's mouth and tongue coordination improves, which will help speech skills
- you burn more calories than usual
- your uterus may shrink toward its pre-pregnancy size more quickly
For more details, see the education sheet "Breastfeeding."
Are there special benefits for a baby with neurological problems?
Breastfeeding helps the baby develop coordination of the muscles and nervous system. The jaw and mouth movements needed for breastfeeding help with this.
The extra closeness and stimulation of being at the breast can enhance the relationship between mother and baby.
What challenges could my baby have with breastfeeding?
An infant with neurological problems usually is either:
- hypotonic (has poor muscle tone)
or - hypertonic (has overreactive muscle tone)
Your infant may tend to:
- have a non-rhythmic suck
- arch the body
- overreact to stimulation
- do too much "rooting"
- bite when swallowing (tonic bite reflex)
- have weak reflexes for sucking, swallowing, and gagging
- get tired more easily: may not nurse long enough to get the hind milk, which has the most calories
How can I help my baby breastfeed?
Feed often (8 to 12 times in 24 hours). You may need to wake your baby to feed. Look for mouth or hand movement even if the baby's eyes are closed. This usually means the infant is in a lighter sleep and can wake up more easily. Other ways to wake the baby: undress for a diaper change, or make skin-to-skin contact.
A baby with low muscle tone usually sucks better when the head and bottom are level, or close to it. Support your baby using pillows on your lap.
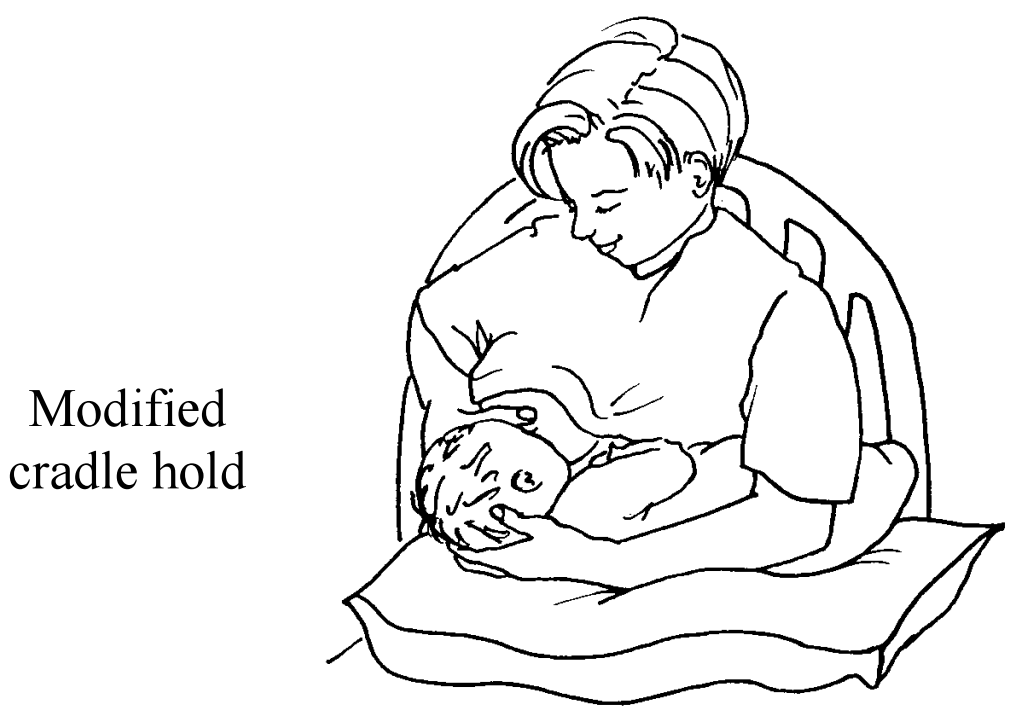
If the infant tends to arch the body, try to hold the infant flexed, with knees bent (as if sitting) and spine rounded. Swaddling in a blanket in a flexed position can help.
If your baby does not start sucking, express some breast milk onto the nipple by hand or use a pump to get "let-down" started. This can encourage the infant to suck.
Try breastfeeding using a sling to keep baby flexed, and to free up your hand to support the chin and jaw.

Once baby starts sucking, look for jaw, ear, and temple movement. If not seen, the infant's suck is probably not as strong as it needs to be.
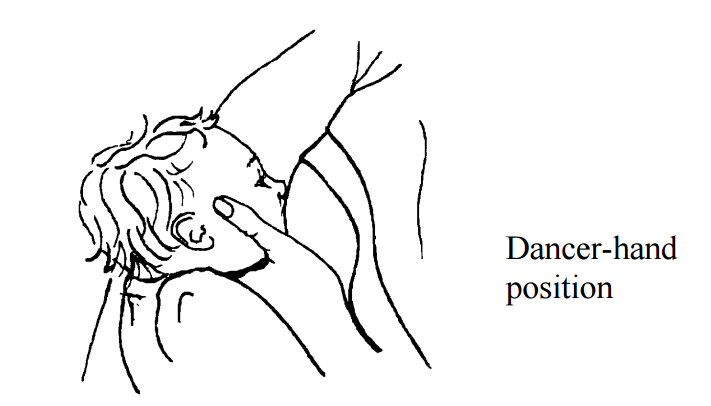
Sometimes the dancer-hand position (see picture below) can be used to support the infant's chin.
Slide the hand under your breast forward, so you are supporting the breast with 3 fingers rather than 4. Form a U-shape with your thumb and forefinger to cradle your baby's chin. This will help your baby press the nipple and areola between the gums.
A breast pump can boost your milk supply while you get started. Feel free to ask your doctor or nurse practitioner.
How will I know if my baby is getting enough milk?
Your baby should nurse every 2 or 3 hours (8 to 12 times in 24 hours), including some feedings during the night.
Watch for this pattern in your baby's urine and stools during the first week after birth:
| Days after birth | Wet diapers (at least this many in 24 hrs) | Stool color | Number of stools (at least this many in 24 hrs) |
| 1st day | 1 | greenish-black | possible stool smears in first 24 hours |
| 2nd day | 2 | 1 to 2 stools | |
| 3rd day | 3 | stool turns yellower, softer, and seedier | 2 to 4 stools |
| 4th day | 4 | 3 to 5 stools | |
| 5th day | 5 | yellow, soft, seedy | 3 to 5 stools |
What else do I need to know?
If the infant has a non-rhythmic suck, try using a rocking chair, and offer extra chin support while breastfeeding.
Breastfeeding in calm surroundings with few distractions can help the infant who easily overreacts to stimulation.
Take care of yourself. You will be spending a lot of time each day feeding your baby. Patience is important.
Get comfortable before starting a feeding. Find a special place—perhaps where you can look out of a window. Cuddle and chat with your baby during each feeding.
Keep what you need at hand—maybe the phone and something to drink. You may want to listen to music or a relaxing program. If you are comfortable and well supported physically and emotionally, you will have more energy to support your baby.
Questions?
This sheet is not specific to you and your baby, but provides general information. If you have any questions, please talk to the nurse or lactation specialist.
At home, if you cannot tell if your baby is getting enough milk, or if you have other concerns, please call the clinic. If you need a pump or a lactation specialist, call:
Hollister at 1-800-323-4060, or
Medela at 1-800-835-5968.
La Leche League, International provides help and support to breastfeeding mothers over the phone and in support groups. For information, call 1-800-525-3243.
Children's Minnesota
Patient/Family Education
2525 Chicago Avenue South
Minneapolis, MN 55404
Last reviewed 8/2015 ©Copyright
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2024 Children's Minnesota
