Nipple Shields
Early latch-on problems are not unusual. For most mothers, breastfeeding takes a bit of practice! Most of the time, a little coaching from a skilled helper is all that is needed to get things going.
For difficult or persistent latch-on problems, many breastfeeding experts suggest the temporary use of a nipple shield. Made of thin, soft, silicone that doesn’t interfere with nipple stimulation, the Medela nipple shield is worn during breastfeeding. Holes at the tip allow milk to flow to the baby. A nipple shield may help protect breastfeeding when:
- The baby is premature, ill, or small. A nipple shield may make feeding easier for a small or weak baby. Because suction inside the nipple shield holds the nipple in an extended position, the baby can pause without ‘losing’ the nipple. Milk pools in the tip of the shield, and provides an immediate reward when the baby resumes suckling. Research shows that the milk intake of premature infants increases when a nipple shield is used. As the baby gains weight and matures, the shield becomes unnecessary.
- The mother has flat or inverted nipples. Some new mothers have nipple tissue that is not very stretchable. If it is difficult for the baby to draw in the mother’s nipple, the baby may pull away, cry, or simply fall asleep. The Medela nipple shield provides sensation deep in the mouth that stimulates the baby to keep sucking. As the milk begins to flow, the baby discovers that breastfeeding works! Over time, the mother’s nipples will become more pliable, and the shield is no longer needed to trigger the sucking reflex.
- The baby has had many bottles and now refuses the breast. Because the nipple shield feels similar to a bottle nipple, it can be used to coax a reluctant baby to accept the breast. Try this trick when the baby is not very hungry and the mother’s breasts are full. Drip a little expressed milk onto the top of the shield to moisten it. Drip milk into the corner of the baby’s mouth to reward the baby for trying. If the milk supply is low, an SNS™ taped under the shield can help provide an encouraging milk flow. Some babies need only a few sessions with a shield to return to full breastfeeding. Other will need more practice, or perhaps brief use of the shield at the beginning of each feed. Bottles can be decreased or discontinued as the baby becomes comfortable with nursing.
WHEN USING A NIPPLE SHIELD:
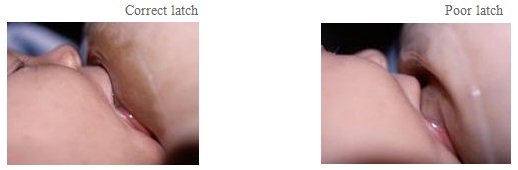
A good latch is especially important when the mother is using a shield. The baby’s jaws must close on the breast, not out on the shaft of the nipple shield. Sucking only on the nipple pinches off the milk flow and fails to stimulate the milk supply. The baby will not get enough milk, and growth may be affected. It helps to have the baby’s latch evaluated by a trained Breastfeeding Specialist.
Cleaning the shield is important.
It is necessary to keep the nipple shield clean. Wash in hot soapy water and rinse in lots of hot water after each use. Boil once daily.
Choosing the correct size shield is important.
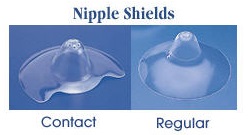
Chose the right size shield for the size of the baby’s mouth. If a shield is too big, the baby cannot adequately draw up the mother’s nipple, or may gag on the shield. The Newborn Small size shield is best for most small babies.. Medela makes several types of nipple shields, the Newborn Small, Newborn Regular, and Contact™ Nipple Shields in two sizes.
Protection of the milk supply is important.
Milk supply is controlled by how much milk the baby takes. A small, weak or poorly suckling baby may under-stimulate the milk supply. When using a nipple shield, it is important to pump after nursing to make sure the breasts are well emptied. Pumped milk can be used to supplement the baby. Pumping after feeding is necessary until it is clear that the milk supply is stable and the baby is growing well. We suggest a hospital quality pump such as the rented Symphony® or Lactina® breastpumps.
Nipple shields are devices that are used to help babies who are not yet breastfeeding normally. Medela, Inc. suggests that mothers using nipple shields seek advice from a lactation consultant or other trained individual, as well as their physicians. Babies should have weight checks frequently to ensure baby’s health and good growth.
Helpful Hints:
Sit the shield on the nipple with the brim turned up like a hat. Then smooth down the edges. This will help the shield stick better. Moistening the edges will also hold it in place. Some mothers have larger nipples than the small shield can accommodate. Try the next largest size. However, observe carefully to see if this size works for the baby. A shield will not solve all problems, and sometimes other equipment may be appropriate.

Weaning from the nipple shield
The nipple shield is a tool to help solve a specific latch problem. They are not a substitute for experienced breastfeeding assistance. If you are using a nipple shield, we suggest that you keep in touch with your lactation professional and your physician as you work to breastfeed comfortably and effectively. The goal is to return to full breastfeeding with no need for special equipment. As the baby’s breastfeeding ability improves, remove the shield at various times during each feeding. If the baby seems unable to nurse without the shield, this means the problem is not yet resolved. Just keep practicing. So long as the baby is growing well, the continued use of the shield is not a major problem. If it appears that the baby could manage without the shield and is using it from habit, some mothers try spending a day in bed with the baby. Quiet time with increased skin-to-skin contact and frequent practicing will reassure the baby that he or she doesn’t really need the shield any more. Cutting away the tip of a silicone is not advised. The cut edges may irritate the baby’s mouth.
By Barbara Wilson Clay, BSEd, IBCLC
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2024 Children's Minnesota
