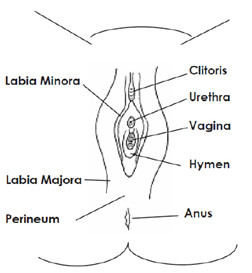
Lichen sclerosus (LIKE-in skler-O-sus) is a skin disorder that affects the vulva (the skin surrounding the vagina). It can happen at any age. It is most common in adults who stopped having their periods (post-menopausal), but can also happen in younger children and teens. In children, it usually appears before menstrual periods start. For some patients, it will go away with periods, but not always, so it is important to follow up with your doctor as directed.
The most common symptoms are itching, irritation, or pain in the skin around the vagina. Sometimes there can be small breaks or “cuts” in the skin that are painful. The way the skin of the vulva looks may also change. Often, the skin looks lighter than the areas around it and may also look thinner, more fragile, or crinkly. Other times, patients may not have any symptoms that they notice.
Often, the lightened area looks like a hourglass or figure of 8 shape around the vulva and anus (where poop comes out). Because the skin is thin, it tears easily, causing pain and bleeding. Bleeding under the skin can cause bright red or purple marks or “blood blisters.” It can also cause pain or burning with peeing or pooping. Women may choose to avoid sex, tight clothing, tampons, riding bikes or horses, and other common activities that involve pressure or friction in the vaginal area.
If lichen sclerosus is not treated or if patients do not follow up as directed, they might get scarring in the vaginal area. The result may be that the inner lips of the vulva shrink and disappear, the clitoris becomes covered with scar tissue, and/or the opening of the vagina may narrow.
If lichen sclerosus is present around the anus it can contribute to constipation (makes it hard to poop). In addition to using the ointment, treatment of constipation is important.
The cause of lichen sclerosus is not completely understood, but an overactive immune system may play a role. There may be a genetic tendency toward the disease. It is not normally due to an infection or trauma.
Lichen sclerosus can be diagnosed in the office by looking at the skin. Sometimes your doctor might need to check a sample of your skin (biopsy) to confirm the diagnosis. A biopsy is usually not necessary.
Lichen sclerosus is a chronic condition that needs ongoing treatment – even if there are no symptoms. Continuing treatment will help prevent symptoms and scarring.
Prescription medicines are required to treat lichen sclerosus. The first treatment of choice is a strong steroid ointment (Clobetasol). Patients use the ointment for about 6 weeks and then their doctor will recheck the area. If things are getting better, the doctor may tell them to use the ointment less often or change to a different ointment. If things are still irritated, patients may continue to use the Clobetasol ointment another 6 weeks. It is important to follow up as scheduled so your doctor can make these changes. Use of these ointments can stop the symptoms (itching and bleeding), help the skin to heal and prevent scarring. Even after the symptoms go away, the medicine should be continued according to your clinicians instructions to prevent scarring and prevent the symptoms from coming back.
Some girls may require lifelong treatment. Lichen sclerosus symptoms may or may not disappear at puberty. Scarring and changes in skin color may not go away even after the symptoms of pain and itching have gone away.
Wear cotton underwear during the day and avoid wearing underwear at night.
This is not specific to your child but provides general information. If you have any questions, please call the clinic.
Reviewesd by GYN 7/2022
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2026 Children's Minnesota