Pulmonary Stenosis
What Is Pulmonary Stenosis?
Pulmonary stenosis (also called pulmonic stenosis) is when the pulmonary valve (the valve between the right ventricle and the pulmonary artery) is too small, narrow, or stiff.
Symptoms of pulmonary stenosis depend on how small the narrowing of the pulmonary valve is. If symptoms are mild, pulmonary stenosis may never require any treatment. But kids with more severe pulmonary stenosis will need a procedure to fix the pulmonary valve so blood can flow properly through the body.
What Happens in Pulmonary Stenosis?
The aortic valve and pulmonary valve control the flow of blood as it leaves the heart and keep it flowing forward. They open to let blood move ahead, then quickly close to keep it from flowing backward. The pulmonary valve lets the blood flow forward to the lungs. It opens to let blood move ahead, then quickly closes to keep blood from flowing backward.
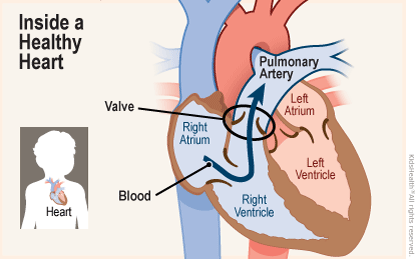
In pulmonary stenosis (pul-muh-NAIR-ee stuh-NO-sis), the pulmonary valve is too small, too narrow, and can't open all the way. This causes the right ventricle to pump harder to send blood out to the lungs. Over time, this can cause thickening of the right ventricle and strain the heart.
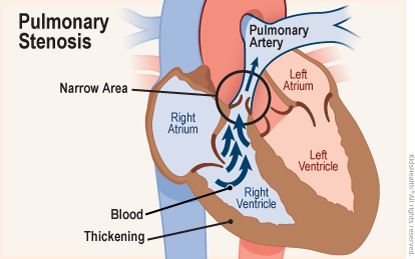
What Are the Signs and Symptoms of Pulmonary Stenosis?
Many people with pulmonary stenosis have no symptoms. Others have mild symptoms that usually don't become bothersome. In most cases of pulmonic stenosis, the doctor will hear a heart murmur.
Symptoms of severe pulmonary stenosis can include:
- in newborns, a bluish tint to the skin (called cyanosis) caused by blood that is low in oxygen
- being very tired
- poor weight gain
- shortness of breath
- palpitations (sensation of rapid or irregular heartbeat)
- chest pain
- fainting
- a swollen abdomen
What Causes Pulmonary Stenosis?
In children, pulmonary stenosis happens when a baby's heart doesn't develop the way it should during pregnancy. Doctors don't know why this happens, but it isn't caused by anything a mother did or didn't do during her pregnancy, so could not have been prevented.
Who Gets Pulmonary Stenosis?
Most cases of pulmonary stenosis are congenital, meaning a baby is born with it.
How Is Pulmonary Stenosis Diagnosed?
Doctors can often identify pulmonary stenosis before birth. This lets babies with severe problems be treated right away.
A fetal echocardiogram (also called a fetal echo) is a type of test that can help diagnose heart defects. A fetal echo uses sound waves to create a moving picture of the heart. This helps doctors see how the baby's heart looks and works while still in the mother's womb.
If the problem wasn't found before birth, infants and older kids who have a suspected heart problem get an echocardiogram. Less commonly, a heart catheterization may be done if a diagnosis isn't clear. In a catheterization, a doctor inserts a catheter (a thin plastic, flexible tube) into an artery and vein that lead to the heart.
How Is Pulmonary Stenosis Treated?
In some cases, pulmonary stenosis doesn't need to be treated. Medicines sometimes can treat symptoms. In severe cases, though, the pulmonary valve will need to be fixed or replaced.
Many types of procedures can repair or replace the pulmonary valve. Most severe cases of pulmonic stenosis can be treated with a balloon valvuloplasty during heart catheterization. With this procedure, a doctor threads an unopened balloon through the pulmonary valve and inflates it to open the valve.
Valve replacement involves using an artificial valve or a valve from a donor.
To decide what treatment to use, doctors consider:
- the location of the narrowing and the amount of narrowing
- the child's age and size
- how well the other valves in the heart are working
- whether the child has had previous heart surgery
- whether the child has other medical conditions
Looking Ahead
A challenge for some kids with pulmonary stenosis is that it can come back again after treatment. This can happen for different reasons, including scar tissue that forms after a procedure or a valve replacement that doesn't grow as kids get bigger. So some kids might need several procedures to keep the valve healthy.
Because pulmonary stenosis can be a lifelong condition, kids who have the defect will need to see a cardiologist (a doctor who specializes in treating heart problems) regularly to make sure the narrowing isn't getting worse.
Many children won't need specific medical treatment, and those who do usually can enjoy most regular activities after their recovery. Kids and teens with moderate or severe pulmonary stenosis should talk with their cardiologist before playing competitive sports or being very physically active.
Note: All information is for educational purposes only. For specific medical advice, diagnoses, and treatment, consult your doctor.
© 1995-2024 KidsHealth ® All rights reserved. Images provided by iStock, Getty Images, Corbis, Veer, Science Photo Library, Science Source Images, Shutterstock, and Clipart.com

