Nosebleeds (Epistaxis)
Article Translations: (Spanish) (Hmong) (Somali)
What causes nosebleeds?
The purpose of the nose is to warm and humidify the air that we breathe in. The nose is lined with many blood vessels that lie close to the surface where they can be injured and bleed. Nosebleeds, can be messy and even scary, but often look worse than they are. Most can be treated at home, but some require medical care.
Common causes of nosebleeds include:
- Dry, heated, indoor air, which dries out the nasal membranes and causes them to become cracked or crusted and bleed when rubbed or picked or when blowing the nose (more common in winter months).
- Colds (upper respiratory infections) and sinusitis, especially episodes that cause repeated sneezing, coughing, and nose blowing.
- Vigorous nose blowing or nose picking.
- The insertion of a foreign object into the nose.
- Injury to the nose and/or face.
- Use of drugs that thin the blood (aspirin, non-steroidal anti-inflammatory medications, and others).
- High blood pressure.
- Tumors or inherited bleeding disorders (rare).
- Nasal or sinus surgery.
How are nosebleeds prevented?
The best treatment of nosebleeds is to prevent them by following these guidelines:
- Avoid nose picking.
- Avoid putting anything hard or solid into the nose.
- Keep the nose moist.
- Use a humidifier in the house, especially the bedroom.
- Use nasal saline spray or nasal saline drops to keep the nose moist. These are available over-the-counter without a prescription. Saline can be used in each nostril 4-6 times daily.
- Use ointment in the nose, such as saline gel or Aquaphor®, or Vaseline®. Make sure it is applied gently, without causing further injury to the inside of the nose.
What should I do if my child gets a nosebleed?
Follow these steps to stop a nosebleed:
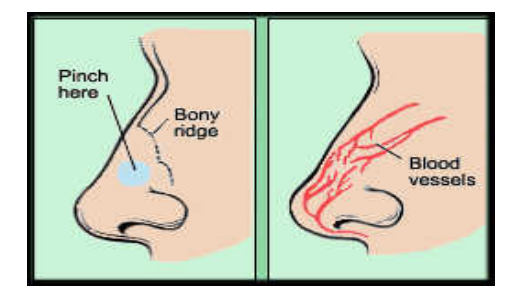
- Have your child sit upright in a chair, with their head up or slightly forward (not tilted back).
- Use a tissue or damp washcloth to catch the blood.
- Use your thumb and index finger to pinch together the soft part of your child's nose just below the nasal bones. Squeezing at or above the bony part of the nose is NOT helpful.
- Keep pinching your child's nose continuously for at least 10 minutes (timed by clock) before checking if the bleeding has stopped. If the nose is still bleeding, continue squeezing the nose for another 10-20 minutes.
- You can spray an over-the-counter decongestant spray, (such as Afrin®, Neo-Synephrine®, others) into the bleeding side of the nose and then apply pressure to the nose as described above. WARNING: These topical decongestant sprays should not be used long term.
- Once the bleeding stops, do not have your child bend over; strain and/or lift anything heavy; and do not blow, rub, or pick the nose for several days.
How are nosebleeds treated?
Treatments, depending on the cause, could include:
- Cauterization – the application of a chemical substance (silver nitrate) or heat energy (electrocautery) to seal the bleeding blood vessel. This is usually done in the operating room, although some older children and teenagers may tolerate chemical cautery in the office with local anesthesia.
- Nasal packing – the placement of gauze or other medical materials into the nasal cavity to stop the bleeding and promote clotting.
- Referral to a hematologist – to test for and treat a bleeding disorder.
When should I call the doctor?
Seek medical care through a physician or an emergency room if:
- You cannot stop the bleeding after more than 20 to 30 minutes of applying direct pressure.
- Your child is experiencing repeated episodes of bleeding.
- The bleeding was caused by an injury to the nose or face.
Questions?
This sheet is not specific to your child but provides general information. If you have questions, please call your doctor or clinic.
Last Reviewed 7/2015 © Copyright
This page is not specific to your child, but provides general information on the topic above. If you have any questions, please call your clinic. For more reading material about this and other health topics, please call or visit Children's Minnesota Family Resource Center library, or visit www.childrensmn.org/educationmaterials.
© 2024 Children's Minnesota
